1. What are common pregnancy discomforts?
– Common discomforts include morning sickness, fatigue, backaches, swollen feet, and mood swings. These are usually part of the normal pregnancy experience.
2. Is spotting during pregnancy normal?
– Light spotting can be normal, especially in the early stages of pregnancy. However, any bleeding should be reported to your healthcare provider for evaluation.

3. How can I manage morning sickness?
– To manage morning sickness, try eating small, frequent meals, staying hydrated, and consuming ginger-based remedies. If it’s severe and affecting your daily life, consult your doctor for additional guidance and possible medication options.
4. What causes heartburn during pregnancy, and how can it be relieved?
– Hormonal changes and the pressure of the growing uterus on the stomach can cause heartburn. To alleviate it, you can eat smaller, more frequent meals, avoid spicy and greasy foods, and consider using antacids or other medications recommended by your healthcare provider.
5. Are headaches common during pregnancy?
– Yes, headaches are common due to hormonal changes and increased blood flow. Rest, proper hydration, and mild, pregnancy-safe pain relievers (consult your doctor) can help manage them.
6. Can I continue to exercise during pregnancy?
– In most cases, yes. Regular, moderate exercise is generally safe during pregnancy and can have several benefits. However, it’s crucial to consult your healthcare provider before starting or continuing any exercise routine to ensure it’s appropriate for your individual situation.
7. Is it normal to have back pain during pregnancy?
– Yes, back pain is common during pregnancy due to the increased weight and changes in posture. You can manage it by maintaining good posture, practicing gentle exercises to strengthen your core and back muscles, and using supportive pillows for sleep.
8. How can I cope with pregnancy-related stress and mood swings?
– Coping with stress and mood swings involves self-care, relaxation techniques, talking to a supportive friend or mental health professional, and getting enough rest. If you experience severe mood swings or depression, seek help from a healthcare provider.
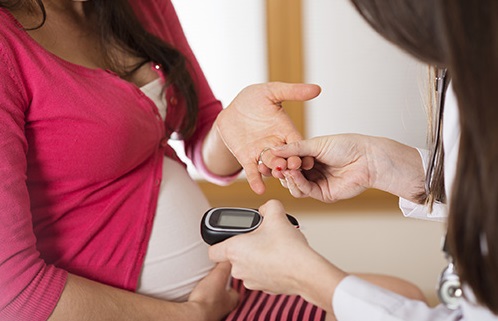
9. What is gestational diabetes, and how is it managed?
– Gestational diabetes is a type of diabetes that usually develops while pregnancy period. It is managed through dietary changes, regular physical activity, and, in some cases, medication prescribed by a healthcare provider. Regular monitoring of blood sugar levels is essential.
10. Are there foods and substances to avoid during pregnancy?
– Yes, pregnant women should avoid raw or undercooked seafood, unpasteurized dairy products, excessive caffeine, alcohol, high-mercury fish, and tobacco. It’s also essential to minimize processed foods and high-sugar items to maintain a healthy diet during pregnancy.
11. What is preeclampsia, and how is it detected and treated?
– Preeclampsia is a severe condition that characterized by high blood pressure and direct effects to organs such as the liver and kidneys. It’s typically detected through regular prenatal check-ups that include blood pressure monitoring and urine tests. Treatment may involve close monitoring, medication, or, in severe cases, inducing labor to prevent complications.
12. Can I travel during pregnancy?
– Travel during pregnancy is generally safe in the early and mid-stages, but consult your healthcare provider before making plans. It’s important to take precautions, stay hydrated, and be aware of any travel restrictions or vaccinations needed. In later stages, travel may become more challenging, so discuss your plans with your doctor.
13. Is it normal to have swollen feet and ankles during pregnancy?
– Yes, mild swelling in the feet and ankles, known as edema, is normal during pregnancy due to increased fluid retention and pressure on blood vessels. To alleviate it, elevate your legs when possible, avoid standing for long periods, and wear comfortable, supportive shoes.
14. Can I continue to work during pregnancy?
– Many women continue to work during pregnancy, but the ability to do so depends on individual circumstances and the nature of the job. Discuss any concerns or adjustments you may need with your employer and healthcare provider, especially if your job involves physical exertion or exposure to hazards.
15. What should I do if I experience severe abdominal pain during pregnancy?
– Severe abdominal pain should not be ignored because it’s contact your healthcare provider immediately, as it could be a sign of a serious issue such as ectopic pregnancy, preterm labor, or a problem with the placenta.
16. Is it normal to experience constipation during pregnancy?
– Yes, hormonal changes and pressure on the intestines can lead to constipation. To manage it, include fiber-rich foods in your diet, drink plenty of water, and discuss safe laxative options with your healthcare provider if needed.
17. How can I prevent stretch marks during pregnancy?
– While it’s challenging to prevent stretch marks entirely, you can help minimize them by staying hydrated, applying moisturizing creams or oils to your belly, and gaining weight gradually within the recommended guidelines.
18. Can I have sex during pregnancy?
– In most cases, sexual activity during pregnancy is safe and healthy. However, it’s essential to communicate with your partner and consult your healthcare provider if you have specific concerns or complications.
19. What is Braxton Hicks contractions, and when should I be concerned about contractions during pregnancy?
– Braxton Hicks contractions are mild, irregular uterine contractions that can occur throughout pregnancy. They are typically harmless and serve as practice contractions. However, if you experience regular, painful contractions before your due date or have concerns about preterm labor, contact your healthcare provider promptly.
20. How do I know when it’s time to go to the hospital for labor?
– It’s time to go to the hospital for labor when your contractions are consistently strong and regular (about five minutes apart), your water breaks, or if you experience heavy bleeding, severe pain, or decreased fetal movement. Contact your healthcare provider for guidance on when to go to the hospital, as it can vary based on individual circumstances.














2 thoughts on “Most Common Problems during Pregnancy (20 FAQs)”